 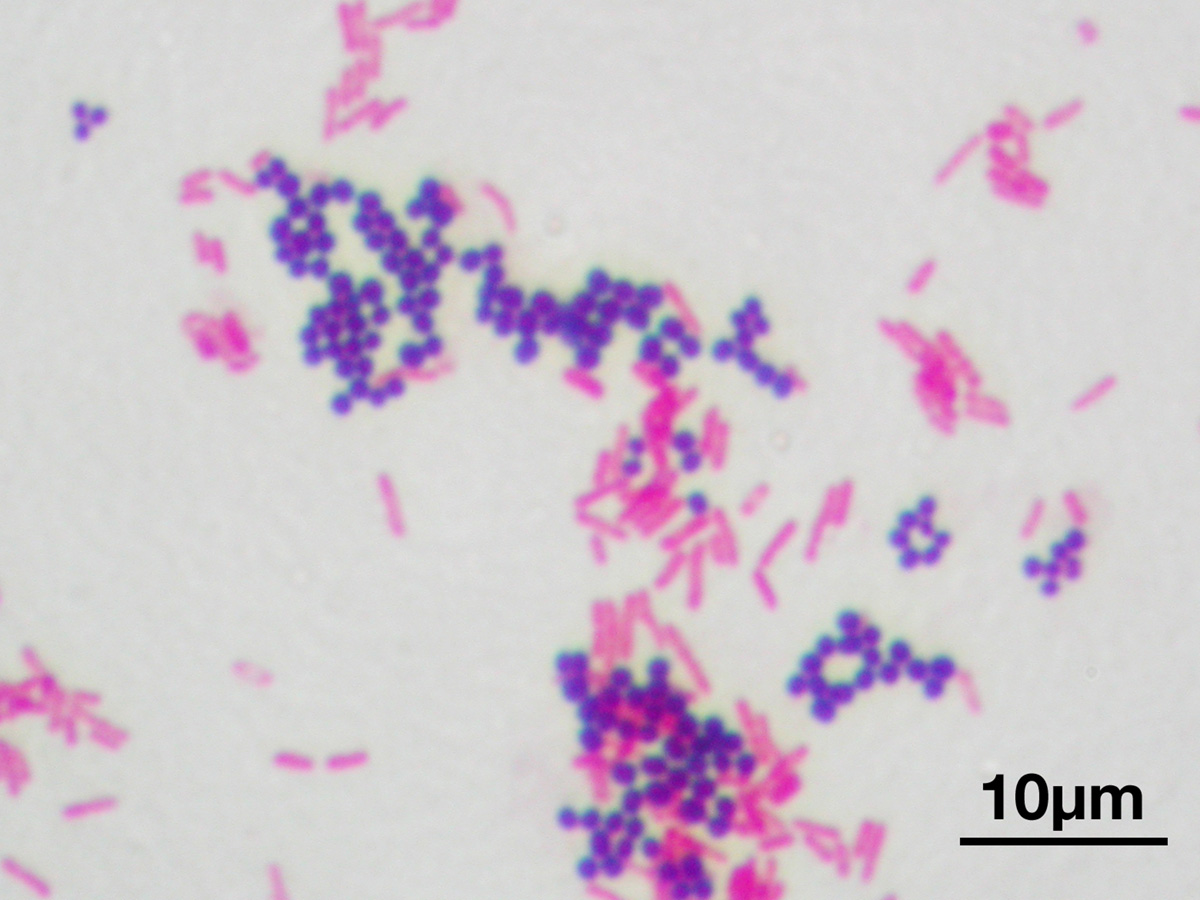
With availability of varies diagnostic modalities for neonatal sepsis such as total blood count, erythrocyte sedimentation rate (ESR), C-reactive protein, platelet count but gold standard is blood culture. Neonatal sepsis present with non-specific signs and symptoms which complicates the clinical diagnosis. Unless proper treatment is not given neonatal septicemia can be life threatening. Among the developed countries the most common cause of neonatal sepsis are Gram-negative pathogens. Over the period of time there is a change in the group of organisms. The pattern of organism in neonatal sepsis among LBW preterm infants is changing constantly. Gram-positive microbes were found to be common pathogens during early periods but later Gram-negative microbes predominated.Īmong neonates systemic infections caused by bacteria occurs due to predisposing factors such as prematurity, premature membrane rupture, poor maternal nutrition, low birth weight, maternal conditions, duration of life support procedures required for postnatal period. A change in the pathogen distribution has been reported by Neonatal Research Network among the low birth weight infants born before 1993 and after 2000. 
Neonatal sepsis with known risk of mortality the survivors of neonatal sepsis had been reported to develop more severe morbidity like pulmonary hypertension, respiratory shock and failure. In a study 35% of mortality was reported among new born with sepsis in low birth weight infants compared to 11% mortality in uninfected low birth weight infants. Among developed countries an incidence rate of 10–25% of LBW preterm infants developing sepsis had been reported. Prolonged hospital stay and central venous catheterization are also other main cause of Neonatal sepsis in LBW preterm infants. LBW preterm infants are more prone for infections mainly because of their underdeveloped immune systems. The causative organisms influence the risk of complication. Neonatal sepsis is a leading cause of morbidity and mortality among low birth weight preterm infants (LBWI). Our study highlights on the surveillance of resistant pathogens causing sepsis in LBW preterm infants emphasizing antimicrobial stewardship to control the mortality rate. The control group showed highest resistance of 62% to the Penicillin group, 54% cephalosporin and 18% for aminoglycosides. Cephalosporin and Penicillin group showed highest resistance with 58 and 52%, respectively. Out of 226 LBW preterm infants 106 (46.9%) showed positive blood culture, of which 52 (49%) Escherichia coli, 28 (26.4%) Klebsiella pneumoniae, 12 (11.32%) Enterobacter spp., 4 (3.7%) Pseudomonas aeruginosa, 2 (1.88%) Acinetobacter spp., 5 (4.7%) methicillin-resistant Staphylococcus aureus (MRSA), 3 (2.8%) Staphylococcus epidermidis were isolated. Antibiotic resistance patterns were performed following standard guidelines. Blood and cerebrospinal fluid (CSF) samples collected for microbiological culture and processed according to standard protocol. A total of 100 normal birth weight infants with sepsis served as control. The study group included 226 LBW preterm infants with sepsis. Neonatal sepsis continues to be a leading and most important cause of mortality among low birth weight (LBW) preterm infants. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
